See how this complicates things whether you want pregnancy or want to avoid it
And yes, stress has something to do with it
In the previous post, I suggested that the terminology that speaks of sub-fertility or reduced fertility is misleading. If you did not stumble over it wondering why, then I am glad for you (I should say, for both of you!). Because you “got it” and you will now think of taking some appropriate steps, and those will NOT be to your insurance agent and/or – more likely – to your bank! (Referencing the high costs of the A.R.T., Artificial Reproductive Technologies.)
Because you understand that, until proven otherwise, your situation should be termed one of instant conceptive gratification cannot be obtained probably due to wrong timing. Nothing reduced or sub- about that! And, the adjective “conceptive” is meant to indicate that the hope is that the other kind of gratification has obtained. The one I referred to as physio-pleasure, but that would be a topic for another time…
Since you are not likely to have reviewed the menstrual variability references given in the previous post, I will document the notion of wrong time with our data. I mean the data from a small clinical trial carried out with a prototype of our core technology, the Ovulona™ for home use.
This trial was performed by an independent group at Marquette University NFP clinic – with patients attending the clinic to learn NFP for one of two reasons: either because they experienced difficulties in achieving pregnancy, or because they wanted to learn NFP [Natural Family Planning] as a means of birth control. Or, maybe, they wanted to use NFP for both, at different phases of their lives.
We can look at data of 10 women, 2 cycles each, reviewing here the ovulation data obtained with said prototype of our Ovulona device.
The data are systematically documented (along with two reference methods for comparison) in the attached 1-page document (Variability of menstrual cycles), and I am doing my utmost to boil it all down for you to as brief a briefing as possible.
Listing of two consecutively detected ovulation days (ovulation marker detected by our device), and noting whether the cycle was subsequently categorized as regular or irregular, goes like this:
Ovulation day number in 2 consecutive cycles
| Patient #1 | 16 (regular) | 17 (regular) |
| Patient #2 | 14 (regular) | 17 (irregular) |
| Patient #3 | 17 (regular) | data absent |
| Patient #4 | 15 (irregular) | 14 (irregular) |
The list goes on, and you should know that “irregular” means “challenged”, and means something of a problem that our modern lifestyle presents to the biology of our women.
One patient provided data from her four cycles, and the variability was – not surprisingly – even more pronounced (-3 days, +3 days, -5 days).
The following table shows the wide spread of the differences between ovulation days in two consecutive menstrual cycles of 10 women attending said NFP clinic.
Summary of 10 patients, 2 consecutive cycles each
|
Patient # |
Ovulation days in 2 consecutive cycles |
Difference between those cycles |
Regular cycles or not |
Age |
Has given birth already or not |
|
1 |
16, 17 |
+1 |
both regular |
35 |
mother |
|
2 |
14, 17 |
+3 |
2nd irregular |
33 |
mother |
|
3 |
17, NA |
NA |
first regular |
42 |
mother |
|
4 |
15, 14 |
-1 |
both irregular |
33 |
mother |
|
5 |
20, NA |
NA |
first regular |
30 |
mother |
|
6 |
19, 18 |
-1 |
both irregular |
38 |
mother |
|
7 |
16, 13 |
-3 |
both regular |
29 |
no children |
|
8 |
21, 24 |
+3 |
2nd irregular |
19 |
no children |
|
9 |
18, 13 |
-5 |
first irregular |
41 |
no children |
|
10 |
10, 12 |
+2 |
2nd irregular |
22 |
no children |
Differences from -5 to +3 days are recorded in this small sample, and the one woman with 4 cycle records showed 5 days difference, too, which illustrates that the more cycles are followed, the larger the spread of ovulation days and cycle lengths usually becomes (this is “cycle irregularity” in the conventional, usual sense).
These are differences between just two successive menstrual cycles. The situation becomes more involved when many more cycles are reviewed, as has been done in the studies years ago using BBT charting data. QUOTE: “The cycle length range was more than five days for 56% of the women who submitted 6 graphs, and for 75% of those with 12 graphs. … Absolute regularity was not demonstrated in as few as six cycles… When the number of cycles was extended to 12, no woman had variability of less than two days in cycle length. END OF QUOTE.
(For reference, go to my previous post at https://biozhena.wordpress.com/2010/03/10/major-studies-decades-ago-revealed-variability-of-menstrual-cycles/ .)
The data of those long-term studies of many menstrual cycles charted by many women are still used today by biostatisticians studying things such as the possibility of sequential predictions of menstrual cycle lengths – the cycle length being primarily dependent on the pre-ovulation part of the cycle (in the absence of any complications).
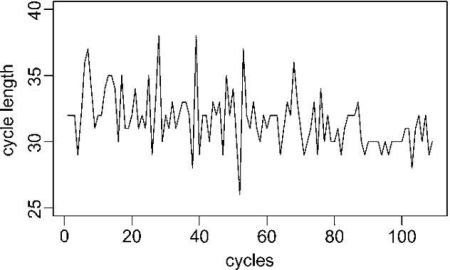
Here is a very good example of cycle length variability of a woman who charted well over a hundred of her menstrual cycles (ref.: Figure 1 http://biostatistics.oxfordjournals.org/content/11/4/741/F1.large.jpg in Paola Bortot, Guido Masarotto, and Bruno Scarpa, “Sequential predictions of menstrual cycle lengths”, Biostat (2010) 11 (4): 741-755 http://biostatistics.oxfordjournals.org/content/11/4/741.full).
I should remind you that our meaning of regularity is as indicated and documented in the attached summary, “Variability of menstrual cycles”. Regular cycles are those where our ovulation marker is within 1 day of LH peak or of the day of Peak mucus (Pk).
Our meaning of irregularity is defined as those cycles where the ovulation marker day data is not within 1 day of said hormone-detecting parameters (LH and estrogen, respectively), and is always higher – signifying delayed ovulation, delayed with respect to the hormonal signals.
As I said above, “irregular” in our parlance means “challenged”, and it means something of a problem that our modern lifestyle presents to the biology of our women. More often than not, the challenge is stress, which I discussed in this blog earlier in at least two posts. Our FIV technology (aka the Ovulona personal monitor) detects the effects of stress, and helps to deal with the consequences in terms of its effect on fertility status.
STOP PRESS
And now, go and check out the 2012 post “The fallacy of ovulation calculators, calendars and circulating-hormone detectors” at https://biozhena.wordpress.com/2012/02/13/the-fallacy-of-ovulation-calculators-calendars-and-circulating-hormone-detectors/
Tags: bioZhena, conception, fertility, ovulation, pregnancy, reproductive
March 29, 2012 at 11:02 am |
[…] About the Added Bonus of Folliculogenesis Monitoring – Automatic Pregnancy Detection Variability of menstrual cycles and of ovulation timing […]
December 14, 2012 at 3:24 pm |
[…] does not stay put on certain days of the menstrual cycle from one cycle to the next. Check out this earlier bioZhena post for evidence that this is so. See evidence generated by other experts years or rather decades ago […]
June 13, 2016 at 8:58 am |
[…] ovulation within those menstrual cycles. For evidence of this variability, see another blog post at https://biozhena.wordpress.com/2010/03/07/variability-of-menstrual-cycles-and-of-ovulation-timing/ (opens in new tab/window). Our focus on the cervix uteri is clarified below in this […]
April 28, 2018 at 3:23 pm |
[…] About the Added Bonus of Folliculogenesis Monitoring – Automatic Pregnancy Detection Variability of menstrual cycles and of ovulation timing […]